Purpose, common side effects…everything you need to know about radiotherapy
By Wokie Passawe
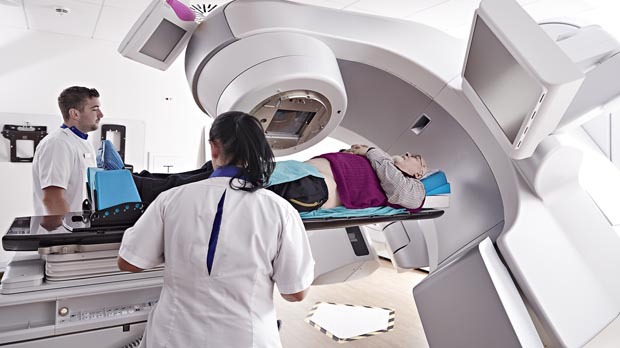
Radiation for cancer treatment, also known as “radiotherapy” is a localized form of treatment that uses high doses of radiation to kill cancer cells and shrink tumors only in the treated area. Radiation can come from a machine or from a small container of radioactive material implanted directly into or near the tumor.
Radiation therapy damages cells by destroying the genetic material that controls how cells grow and divide. While both healthy and cancerous cells are damaged by radiation therapy, the goal of radiation therapy is to destroy as few normal, healthy cells as possible. Radiation can be used to treat just about every type of cancer and is also found useful in treating some noncancerous (benign) tumors.
Pros: ● Can target and kill a large portion of cancer cells (within the tumor)
- Can shrink a tumor in preparation for surgery
- Relatively safe
- Painless (you cannot actually “feel” radiation as it is happening)
- Does not require anesthesia
- Preserves the organ that developed the cancer (i.e. breast will remain intact)
Cons: ● Cannot be used to treat cancer that has spread to other places in the body
- Damage to surrounding tissue(s)
- Cannot target / kill cancerous cells that cannot actually be seen on on an imaging screen
- When a tumor is large it may not kill all cancer cells
- Wound complication / poor healing at times in the area that received the radiation
- Skin radiated can become red, tender and peel
- Possible fatigue
- Inconvenient (in most cases it is delivered 5 days per week over a period of time).
WHEN RADIATION IS COMBINED WITH SURGERY
Radiation can be performed prior to surgery (pre-operative) or after surgery (post-operative) and both have their pros and cons. The outcome of which your doctor suggests is dependent on characteristics of the tumor and the patient themselves. Radiation is typically and strongly recommended for women who had positive lymph nodes.
Preoperative Radiation Therapy:
Preoperative Pros: can shrink the tumor prior to surgery, lowers risk of local recurrence and distant metastases.
Preoperative Cons: possibly obscures the extent of the tumor due to shrinkage and destruction of the margins of the tumor and can increase postoperative complications.
Postoperative Radiation Therapy:
Postoperative Pros: can eliminate any tumor cells that still remain after surgery, reduces the occurrence of the cancer re-developing at the same site. Postoperative Cons: possibly obscures the extent of the tumor due to shrinkage and destruction of the margins of the tumor and can increase postoperative complications.
Overall, there are 2 goals with radiotherapy:
1) Cure – get rid of the cancer completely, and hopefully prevent the cancer from returning.
2) Alleviate – to make symptoms better and improve your quality of life more specifically for patients whose cancer has spread beyond their breast to different parts of the body.
Common side effects:
Note: Side effects can be treated and controlled. They are not permanent.
1) Fatigue
2) Skin reactions (rash or redness)
3) Loss of appetite
4) Decrease number of white blood cells
5) Inflammation of tissues and organs in the site that is radiated
Other things to know:
1) Who will administer your radiotherapy? A radiation oncologist
2) Will you start the same day you meet your radiation oncologist? Likely not, but probably within days following.
3) Should I eat anything in particular while undergoing radiotherapy? There are no food/diet restrictions. Continue to make health(ier) choices. If you have any other health concerns, your team may add restrictions.
4) What does it feel like? You cannot feel radiation. It’s like getting an x-ray, except directed towards the tumor.
5) Am I awake during radiation? Yes, you will be awake.
6) Will I be radioactive during or after treatments? No, patients are not radioactive during or after external radiation therapy.